For decades, cholecystectomy has been the standard treatment for gallstones, based on the idea that removing the gallbladder eliminates the disease. While effective, this approach is not without drawbacks. The gallbladder plays an important physiological role in bile storage and controlled release, and its removal can lead to long-term digestive disturbances in some patients.
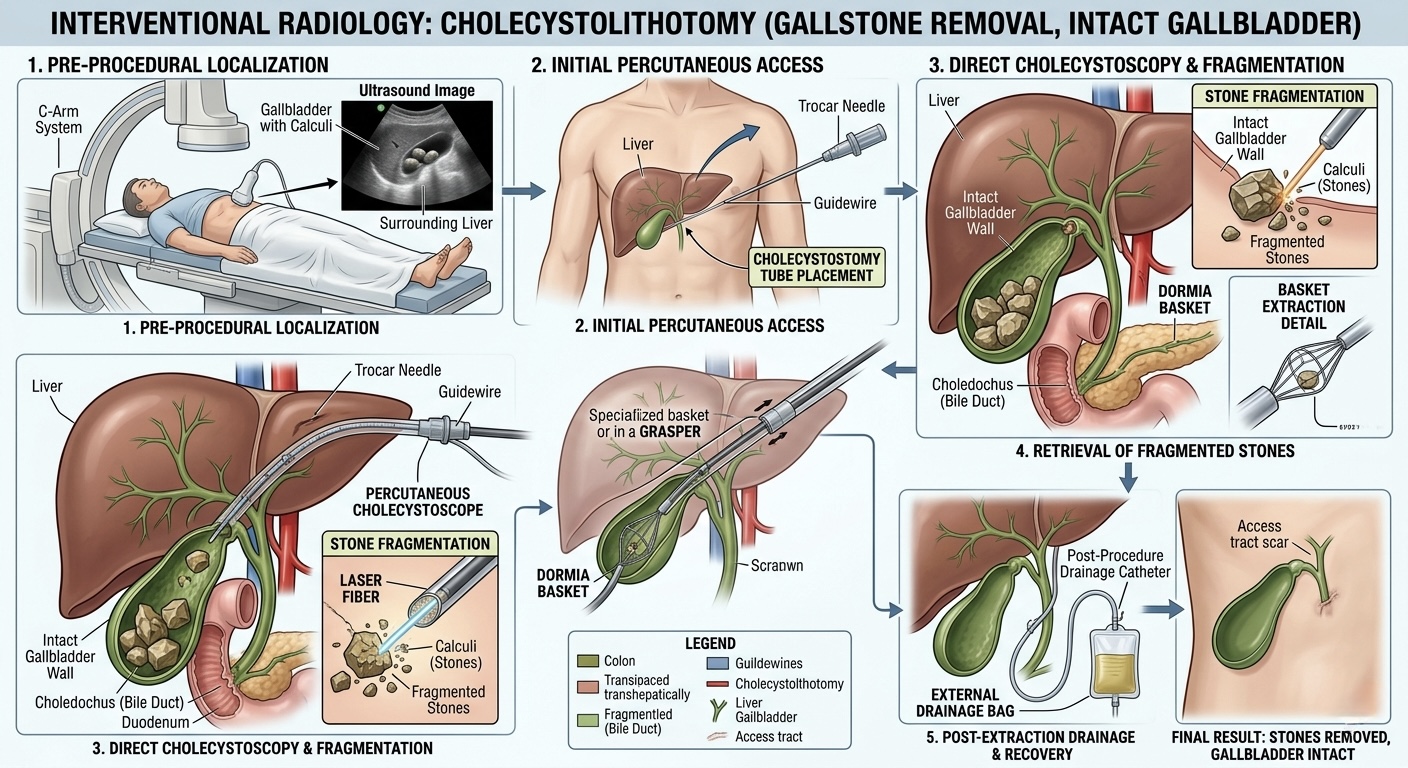
Interventional radiology is now introducing a shift in this long-standing paradigm. A minimally invasive technique known as Percutaneous Cholecystolithotomy (PCCL) focuses on removing only the gallstones while preserving the gallbladder. Under image guidance, a small tract is created into the gallbladder, allowing instruments to fragment and extract the stones without the need for major surgery. The organ remains intact, maintaining its natural function.
This approach offers several advantages. Patients experience less pain, shorter hospital stays, and quicker recovery compared to traditional surgery. More importantly, preserving the gallbladder helps maintain normal digestive physiology, potentially avoiding the post-cholecystectomy symptoms seen in some individuals. It is particularly beneficial for patients who are high-risk surgical candidates, such as the elderly or those with significant comorbidities.
Although concerns like stone recurrence and careful patient selection still limit its widespread adoption, ongoing advancements in imaging, instrumentation, and technique are steadily improving outcomes. As interventional radiology continues to evolve, procedures like PCCL represent a future where organ preservation becomes the priority rather than removal.
Cholecystectomy is still widely practiced today, but its dominance is being challenged. The future of gallstone management is moving toward safer, less invasive, and more physiologically sound treatments—and interventional radiology is at the center of this transformation.





